Nursing Maldistribution: The Intersection Between Practice Setting and Years of Nursing Experience
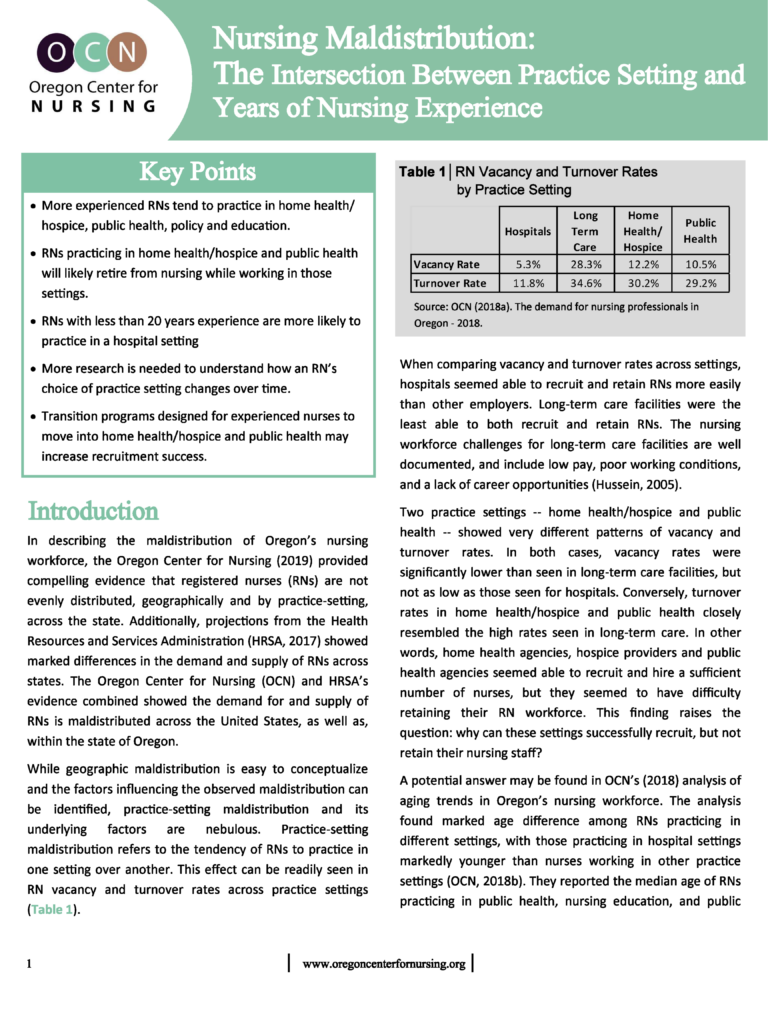
RNs across Oregon are not evenly distributed between care settings, especially when considering years of experience. Nurses with more experience tend to cluster in non-hospital environments, while newer nurses gravitate toward hospitals and long-term care. These patterns raise important implications for workforce planning, recruitment, and retention strategies statewide.
Primary Care Workforce Crisis Looming in Oregon: Nurse Practitioners Vital to Filling the Gap, But Not Enough to Go Around

Oregon faces an urgent primary care shortage, with only a fraction of nurse practitioners delivering direct primary care services. Despite favorable practice laws, the state struggles to align NP capacity with community needs. Policymakers must rethink workforce distribution to avoid deepening care disparities statewide.
Trends in Oregon Nursing Education 2012–18

Nursing education in Oregon is evolving, but not fast enough to meet projected workforce needs. While BSN programs are growing, ADN and LPN pathways show stagnation or decline. This analysis highlights long-term trends shaping the state’s ability to “grow its own” nursing workforce.
Shortage or Maldistribution: Shifting the Conversation About Oregon’s Nursing Workforce

Misconceptions about a statewide nursing shortage often overshadow a more pressing issue: maldistribution. This analysis reveals how workforce imbalance affects rural regions and non-hospital settings. OCN’s research encourages targeted action by identifying critical disparities in nurse availability across Oregon.
Nursing Apprenticeships: Examples for Oregon Discussion

Nursing apprenticeships are gaining renewed attention as a strategy to address workforce shortages in healthcare. This discussion paper explores existing models and evaluates their relevance to Oregon’s nursing pipeline. It invites healthcare leaders and policymakers to reimagine how education and on-the-job training can work together.
The Demand for Nursing Professionals in Oregon – 2018

Employer perspectives across Oregon’s healthcare sectors reveal rising turnover and vacancy rates, especially in long term care. Survey findings uncover how workforce challenges vary dramatically across hospitals, public health, home health, and hospice settings. With regional shortages looming, employer responses suggest that targeted, sector-specific strategies are critical to stabilize Oregon’s nursing pipeline.
2018 Aging Trends in Oregon’s Nursing Workforce

Oregon’s nursing workforce is getting younger, with a growing presence of nurses in their 20s and 30s. While this demographic shift offers promise, it raises urgent questions about experience gaps and impending retirements. This analysis explores how age trends differ by geography and employment setting, and what they mean for Oregon’s healthcare system.
Characteristics of the Nursing Workforce in Oregon – 2016

Nurses make up the largest share of Oregon’s healthcare workforce, serving as essential contributors to care access, quality, and cost outcomes. This 2016 profile outlines age, education, gender, and licensure trends across practice settings and specialties. Workforce planners, educators, and employers will find critical context for responding to statewide healthcare demands.
Nursing Education in Oregon (2016)
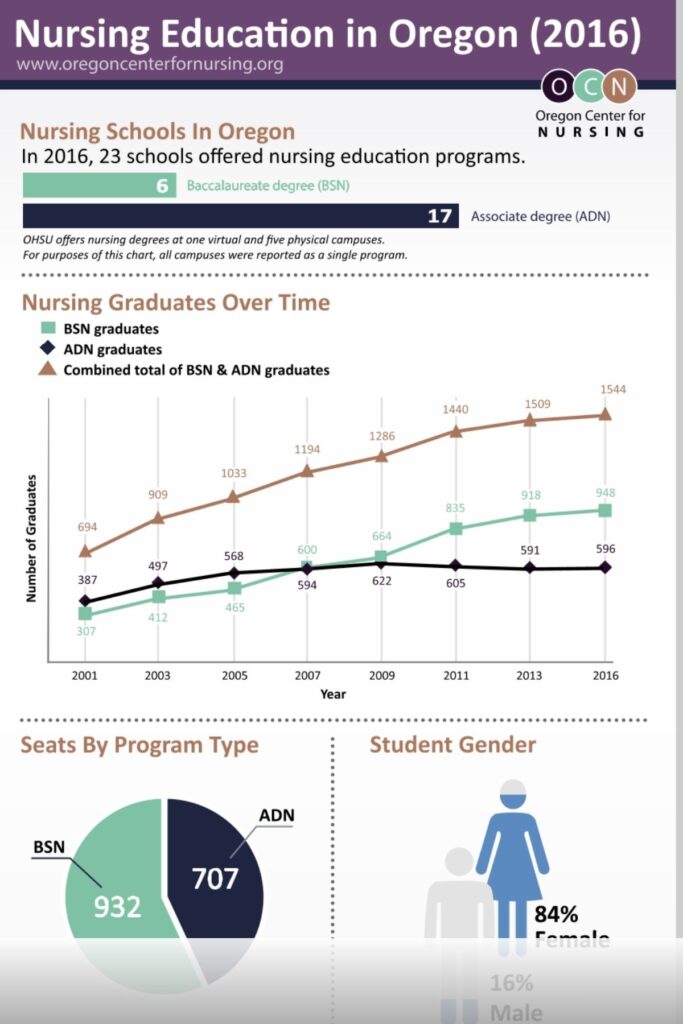
Explore the 2016 landscape of Oregon’s nursing education programs through a visual breakdown of graduates, gender ratios, and program distribution. This concise infographic helps illuminate workforce trends across ADN and BSN programs. It’s a valuable snapshot for educators, employers, and policymakers.
Oregon Nurse Faculty: Why Are They Leaving?

Oregon’s nursing education system faces a growing challenge: faculty are leaving their positions at concerning rates. This publication explores the key factors behind their departure, including workload, compensation, and institutional support. Understanding these trends is essential to ensuring the future stability of Oregon’s nursing workforce.
