From Burnout to Belonging: Nurse-Designed Approaches to Workforce Well-Being in Oregon

What happens when nurses design the solutions to their own workplace stress? Across Oregon, 18 nurse-led initiatives did just that, reshaping care environments and reframing well-being from the inside out. Discover how voice, equity, and system-level design replaced quick fixes and built lasting change.
Oregon Healthcare Workforce Index: Understanding Nursing in the Broader Healthcare Labor Market

Nursing shortages don’t happen in isolation as they reflect deeper workforce dynamics. This index reveals how interconnected roles like medical assistants, respiratory therapists, and advanced practitioners impact Oregon’s nursing workforce. Built from public employment and wage data, the tool offers a new lens for planning healthcare workforce strategies across the state.
Comparison of the Perception of Clinical Instruction: In-Facility, Face-to-Face Simulation, and Virtual Simulation Experiences in Oregon’s Nursing Programs

Simulation-based instruction has become a key tool in Oregon’s nursing education, especially during pandemic-era disruptions. This study explores how students and faculty perceive in-facility, face-to-face, and virtual simulation methods. Findings reveal notable differences between student and faculty viewpoints across instructional environments.
Filling the Gap: An Examination of Oregon Registered Nurses Licensed Through Endorsement

Oregon’s growing nurse demand increasingly depends on nurses licensed through endorsement. This report explores where these nurses practice and how that impacts healthcare access. Insights reveal how rural and non-hospital settings may face widening staffing gaps if current trends persist.
Issues Facing the Post-Pandemic Nursing Workforce in Oregon – Lasting Pandemic Impacts

Oregon’s nursing workforce is still grappling with lingering effects of the COVID-19 pandemic, from license disruptions to emergency staffing shifts. This report explores how short-term policy responses and long-term workforce trends are reshaping the profession. As the state navigates a post-pandemic future, key questions remain about staffing capacity and nurse retention.
Not Working Well: Clinical Placement for Nursing Students in an Era of Pandemic

Faced with the urgency of a global health crisis, nursing education programs and healthcare agencies in Oregon scrambled to adapt clinical placement strategies. This publication captures the resulting stress, innovation, and breakdowns that surfaced as traditional education pipelines were upended. Interviews across sectors reveal a critical moment of reckoning for how students are prepared for practice.
Issues Facing the Post-Pandemic Nursing Workforce in Oregon

COVID-19 intensified Oregon’s existing nursing workforce challenges, disrupting education pipelines and stressing care delivery systems. This report explores how these shifts affect nurse training, licensure trends, and frontline well-being. Nurse migration patterns and burnout risks reveal vulnerabilities that require immediate and strategic attention.
The Nurse Licensure Compact – a Primer

Debates around the Nurse Licensure Compact continue as states weigh the benefits of streamlined licensing against regulatory concerns. This primer explains the NLC’s mechanisms and outlines the arguments made in Oregon’s policy discussions. With multi-state licensure on the rise, understanding its implications remains vital for nursing leadership.
Nursing Maldistribution: The Intersection Between Practice Setting and Years of Nursing Experience
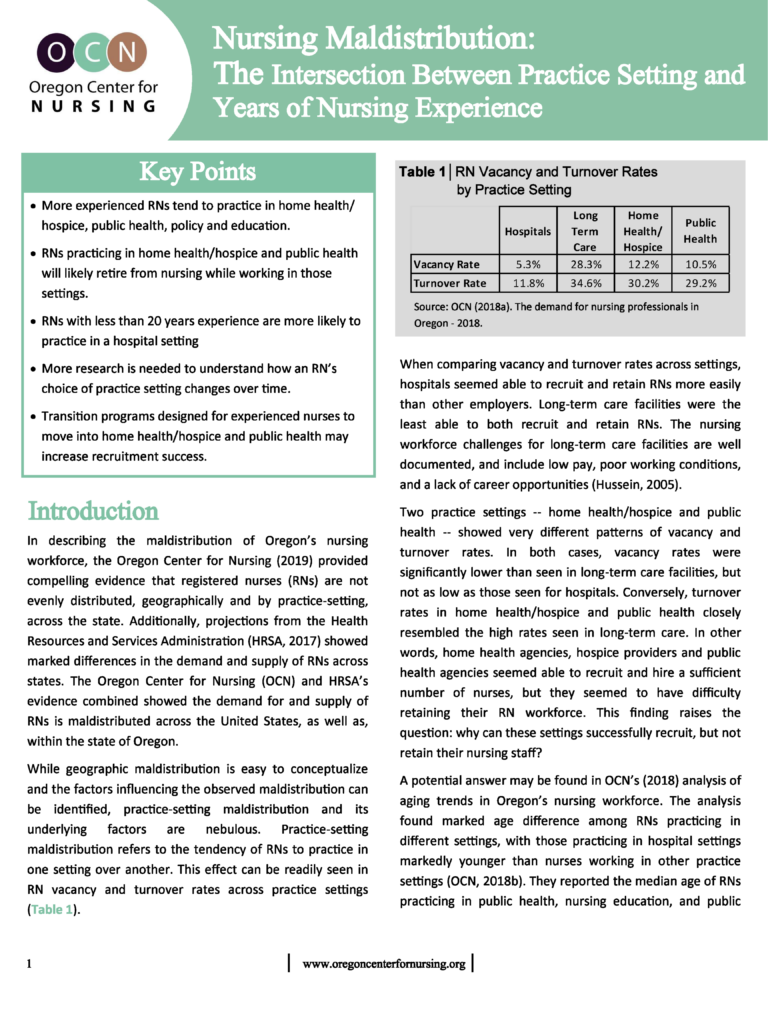
RNs across Oregon are not evenly distributed between care settings, especially when considering years of experience. Nurses with more experience tend to cluster in non-hospital environments, while newer nurses gravitate toward hospitals and long-term care. These patterns raise important implications for workforce planning, recruitment, and retention strategies statewide.
Primary Care Workforce Crisis Looming in Oregon: Nurse Practitioners Vital to Filling the Gap, But Not Enough to Go Around

Oregon faces an urgent primary care shortage, with only a fraction of nurse practitioners delivering direct primary care services. Despite favorable practice laws, the state struggles to align NP capacity with community needs. Policymakers must rethink workforce distribution to avoid deepening care disparities statewide.
